HSG Study Finds Healthcare Executives Took Measures to Prevent Decreased Provider Compensation Despite Decreased Patient Volume
LOUISVILLE, Ky., October 15, 2021 (Newswire.com) - With the number of employed physicians continuing to grow throughout the pandemic, hospitals and healthcare organizations had to explore strategies to address employed provider compensation. To gain a better understanding of how growing employment, changes to the 2021 Medicare Physician Fee Schedule (MPFS) and COVID-19 impacted provider compensation, HSG, a national healthcare consulting firm, has published a white paper examining the results of their own healthcare executive survey.
"We wanted to provide in-depth analysis of these two issues and discuss strategies that healthcare leaders can take to avoid potential pitfalls related to provider compensation," said Eric Andreoli, Director at HSG. "Regardless of how your organization implements the updated Medicare fee schedule, it is critical to be aware of the long-term impact each decision point can have on your health system's financial status."
Two acute issues continue to add challenges to provider compensation. First, reduced patient volume during the COVID-19 pandemic leading to artificially high per wRVU compensation rates in surveys based on 2020 data. Second, for many specialties, changes to the 2021 MPFS resulting in wRVU production that is significantly higher than levels reported in surveys using data from prior years. Despite decreasing patient volume, many organizations took steps to protect provider compensation.
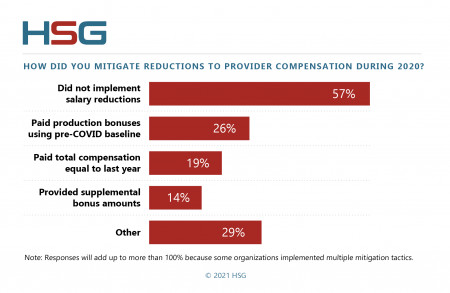
In August of 2021, HSG asked 68 healthcare executives from across the country to comment on their organization's 2020 provider compensation challenges during, and in response to, the COVID-19 pandemic. More than 90% of these organizations utilize provider compensation plans that include components tied to wRVU production. Recognizing that a drop in wRVUs would lead to decreased provider compensation, many organizations took measures to mitigate the impact of reduced patient volume. In fact, 83% of the executives surveyed indicated implementing mitigation measures. The most common approaches included not implementing reductions and/or paying providers based on pre-COVID productivity levels.
Despite these mitigation measures, approximately half of these executives indicated a negative impact to their providers' compensation. This impact varied by specialty type, with surgeons more likely to see a decrease in compensation and some hospital-based physicians seeing an increase to compensation. APPs were less likely to be impacted since a majority of these providers are typically on base salary models.
"Due to the complexity surrounding these compensation issues, we see many organizations continuing to use the 2020 MPFS to calculate wRVUs for production-based provider compensation plans. In the short term, this ensures providers will continue to earn at current compensation levels for current volume. This also gives organizations time to conduct analysis and develop a strategy for adjusting compensation parameters to coincide with 2021 MPFS implementation," stated Andreoli.
For many healthcare organizations and hospitals, overcoming challenges in provider compensation means redesigning elements to better align with organizational goals and objectives. HSG partners with clients on an ongoing basis to overcome challenges with provider compensation. This may involve focusing on alignment between productivity and compensation, balancing market rates with organizational sustainability, and/or shifting compensation dollars towards value. To better understand the issues at hand, read the white paper and gain access to additional data points uncovered by HSG's most recent executive survey, visit the website at HSGadvisors.com/thought-leadership/.
###
About HSG
HSG builds high-performing physician networks so Health Systems can address complex changes with confidence. HSG, a Louisville-based, national healthcare consultancy firm, can be reached via their website, LinkedIn, by emailing info@hsgadvisors.com, or by calling (502) 814-1180.
Media Contact: Karolyn Raphael, karolyn@wingermarketing.com
Source: HSG
